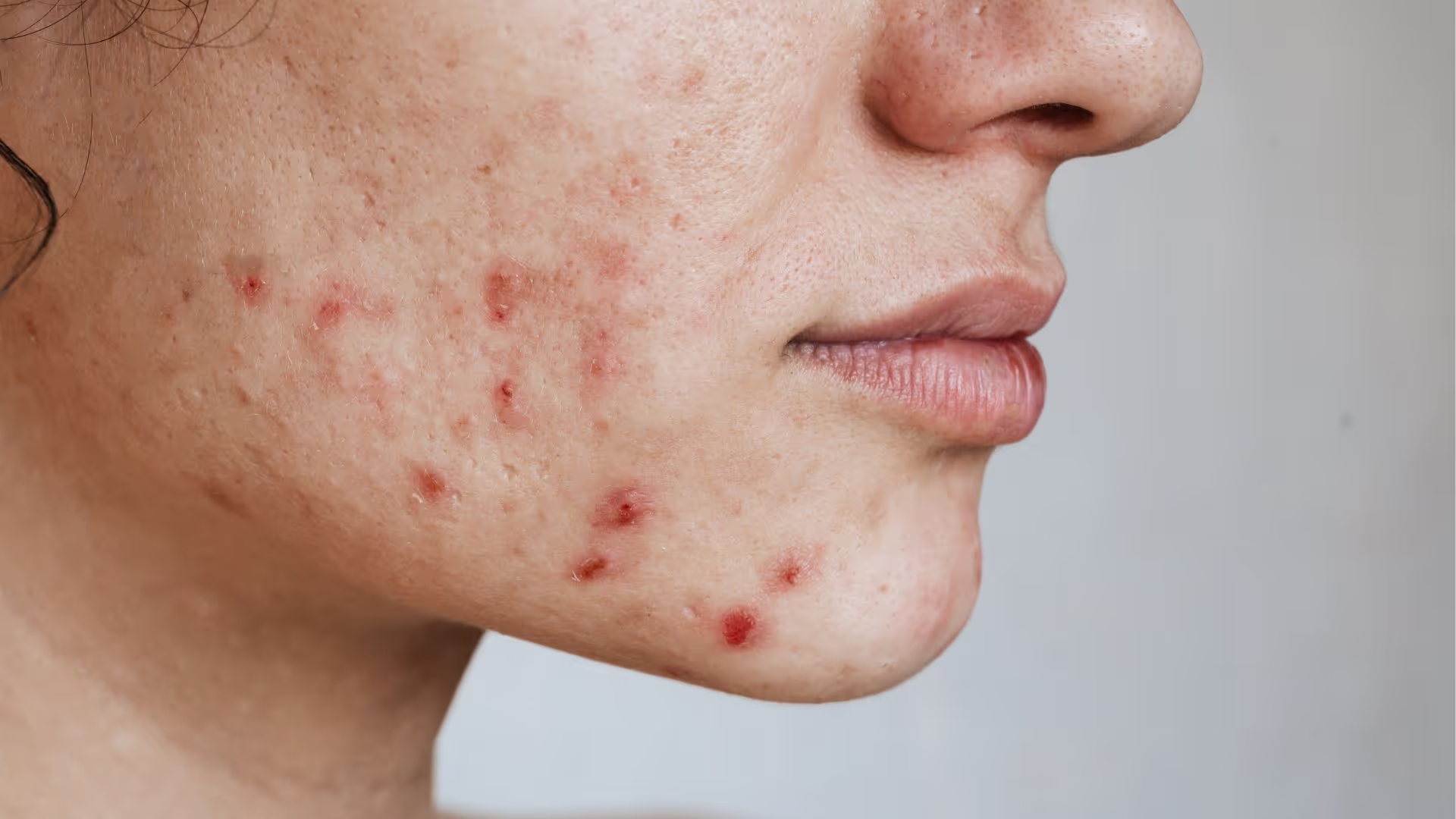
Fungal Acne vs. Regular Acne: Understanding Your Breakouts
Dealing with persistent skin breakouts can be incredibly frustrating. You cleanse, you treat, and yet those stubborn bumps just won't budge. While many assume all pimples are "acne," the truth is your skin might be battling a completely different foe. This often-misunderstood adversary is known as fungal acne, and mistaking it for regular bacterial acne can lead to ineffective treatments and ongoing discomfort. Understanding the distinct differences between these two conditions is the first crucial step towards achieving clear, healthy skin, and it fundamentally impacts why your choice of cleanser matters more than you think.
The Unseen Culprit: What Exactly is Fungal Acne?
The term "fungal acne" itself is a bit of a misnomer, contributing to much of the confusion surrounding the condition. Scientifically known as Malassezia folliculitis or Pityrosporum folliculitis, it isn't acne in the traditional sense, but rather an infection of the hair follicles caused by an overgrowth of yeast. Specifically, a type of yeast called Malassezia (which naturally lives on everyone's skin) proliferates, feeding on the excess sebum (oil) your skin produces. This overgrowth leads to the characteristic breakout of small, often itchy, bumps.
Unlike bacterial acne, which results from clogged pores, excess sebum, and the proliferation of bacteria like P. acnes, fungal acne thrives in specific conditions. It is frequently triggered by:
- Humid Environments: Yeast loves warmth and moisture.
- Excessive Sweating: Especially after workouts or in hot climates.
- Tight or Occlusive Clothing: Traps heat and moisture against the skin.
- Broad-Spectrum Antibiotics: These can inadvertently kill off beneficial bacteria that keep yeast in check, allowing Malassezia to flourish.
- Oil-Based Skincare Products: Certain oils can provide a food source for the yeast.
- Compromised Skin Barrier: A weakened barrier can make the skin more susceptible to yeast overgrowth.
While traditional acne typically appears on the face, fungal acne commonly affects the chest, back, shoulders, and even the arms, though it can certainly manifest on the face too. It's important to dispel the myth that fungal acne is a sign of poor hygiene; it's an imbalance in your skin's natural microflora, not a cleanliness issue.
Related Malassezia-Driven Skin Conditions
The Malassezia yeast is also implicated in other common skin conditions, which can sometimes coexist with or be mistaken for fungal acne:
- Seborrheic Dermatitis: Characterized by flaky, red, sometimes greasy patches on oily areas like the scalp, eyebrows, sides of the nose, and chest. It's essentially dandruff on other parts of the body.
- Tinea Versicolor: A fungal infection that causes discolored patches on the skin, often lighter or darker than the surrounding skin, and may appear scaly.
Understanding these connections highlights just how prevalent Malassezia-related issues can be and why a targeted approach is so vital.
Spotting the Difference: Fungal vs. Regular Acne
Differentiating between fungal acne and regular bacterial acne is paramount for effective treatment. Treating fungal acne with conventional acne remedies not only wastes time and money but can often worsen the condition by further disrupting the skin's natural balance or providing more "food" for the yeast.
Here’s a breakdown of key indicators to help you distinguish between the two:
Symptoms of Fungal Acne (Malassezia Folliculitis):
- Appearance: Typically presents as small, uniform, pinprick-sized bumps (papules and pustules). They often look like tiny whiteheads.
- Itchiness: This is a major distinguishing factor. Fungal acne is almost always intensely itchy, a sensation rarely associated with bacterial acne.
- Location: While it can appear anywhere, it's very common on the chest, back, shoulders, and hairline. When on the face, it often concentrates around the T-zone or areas where sweat accumulates.
- Response to Treatment: Often resistant to traditional acne treatments like benzoyl peroxide or salicylic acid. May even worsen after using antibiotics or oil-rich moisturizers.
- Uniformity: The bumps tend to be similar in size and shape, often clustered together.
Symptoms of Regular (Bacterial) Acne:
- Appearance: Varies greatly, including blackheads, whiteheads, papules, pustules, cysts, and painful nodules.
- Itchiness: Generally not itchy, though severe inflammatory cysts can be painful or tender to touch.
- Location: Most common on the face, but also appears on the neck, chest, back, and shoulders.
- Response to Treatment: Typically responds to conventional acne treatments containing ingredients like salicylic acid, benzoyl peroxide, retinoids, or topical antibiotics.
- Variability: Bumps can be of different sizes and types within the same breakout area.
If you suspect you have fungal acne, especially if your breakouts are itchy, uniform, and haven't responded to standard acne treatments, it's crucial to reconsider your approach. While these guidelines can help, always consult a dermatologist for an accurate diagnosis.
Why Your Cleanser is the Game Changer: The Power of an Anti Fungal Face Wash
Given the distinct nature of fungal acne, it becomes clear why your choice of cleanser is not just important, but absolutely critical. Using a regular acne cleanser, even one designed for "blemishes," might contain ingredients that aggravate fungal acne by further irritating the skin or, paradoxically, feeding the yeast. For instance, some oil-based cleansers or those with certain fatty acids can act as a nutrient source for Malassezia.
This is where an Anti Fungal Face Wash comes into its own. These specialized cleansers are formulated with active ingredients specifically designed to inhibit the growth of yeast and restore balance to your skin's microflora. When searching for an effective solution, look for ingredients such as:
- Ketoconazole: A powerful antifungal agent commonly found in prescription and over-the-counter washes and shampoos. It works by disrupting the yeast's cell membranes.
- Selenium Sulfide: Another effective antifungal and anti-seborrheic agent that helps reduce yeast on the skin and control oil.
- Zinc Pyrithione: Known for its antifungal and antibacterial properties, it's often used in dandruff shampoos and is highly effective against Malassezia.
When selecting an Anti Fungal Face Wash, it's also vital to ensure it is:
- Fungal Acne Safe: This means the product's ingredients have been checked and are unlikely to feed Malassezia yeast. Many online resources and apps can help you verify ingredient lists.
- Non-Comedogenic: While fungal acne isn't about clogged pores, non-comedogenic products are generally less likely to irritate sensitive, compromised skin or contribute to any coexisting bacterial acne.
- Gentle and pH-Balanced: Harsh cleansers can strip your skin's natural barrier, making it more vulnerable. A gentle, pH-balanced formula supports barrier health.
Practical Tips for Using an Anti Fungal Face Wash:
- Consistency is Key: Use your Anti Fungal Face Wash regularly, often twice daily, as directed by product instructions or a dermatologist.
- Allow Contact Time: Unlike a quick rinse, many antifungal washes benefit from being left on the skin for a minute or two before rinsing. This allows the active ingredients to work effectively.
- Patch Test: Always perform a patch test on a small, inconspicuous area of your skin before applying a new product to your entire face or body, especially if you have sensitive skin.
- Complementary Skincare: Ensure the rest of your skincare routine (toners, serums, moisturizers) is also fungal acne-safe to avoid counteracting the benefits of your specialized cleanser. Look for ingredients lists that avoid esters and polysorbates, which can feed Malassezia.
- Shower Immediately After Sweating: If intense physical activity or humid conditions trigger your fungal acne, use your Anti Fungal Face Wash or body wash immediately after sweating.
Beyond the Cleanser: Holistic Management for Clear Skin
While an Anti Fungal Face Wash is a cornerstone of treatment, managing fungal acne effectively often requires a holistic approach:
- Breathable Fabrics: Opt for loose-fitting clothing made from natural, breathable materials like cotton, especially during workouts or in warm weather.
- Dietary Considerations: Some individuals report improvements by reducing sugar and refined carbohydrates in their diet, as yeast thrives on sugar. While not scientifically proven for skin application, it's a common anecdotal approach.
- Hydration: Keeping your skin properly hydrated with fungal acne-safe moisturizers can help support a healthy skin barrier.
- Professional Guidance: If over-the-counter solutions aren't providing relief, a dermatologist can offer stronger prescription antifungal medications (topical or oral) and personalized advice. They can also confirm the diagnosis, ruling out other conditions.
Conclusion
The journey to clear skin begins with accurate identification. Understanding that your "acne" might actually be fungal acne is a pivotal moment, shifting your treatment strategy from frustration to targeted effectiveness. By recognizing the tell-tale signs of Malassezia folliculitis and embracing the power of a specifically formulated Anti Fungal Face Wash, you can effectively combat this persistent condition. Pair the right cleanser with a comprehensive, fungal acne-safe skincare routine and lifestyle adjustments, and you'll be well on your way to soothing those itchy bumps and revealing the radiant skin you deserve.